Impression Techniques
Place tip of the tongue to the soft palate. Practice biting on the second molars (pretend if not present). Goal is to get condyles in the TMJ fossae to rotate in their correct orthopedic position.

Place tip of the tongue to the soft palate. Practice biting on the second molars (pretend if not present). Goal is to get condyles in the TMJ fossae to rotate in their correct orthopedic position.
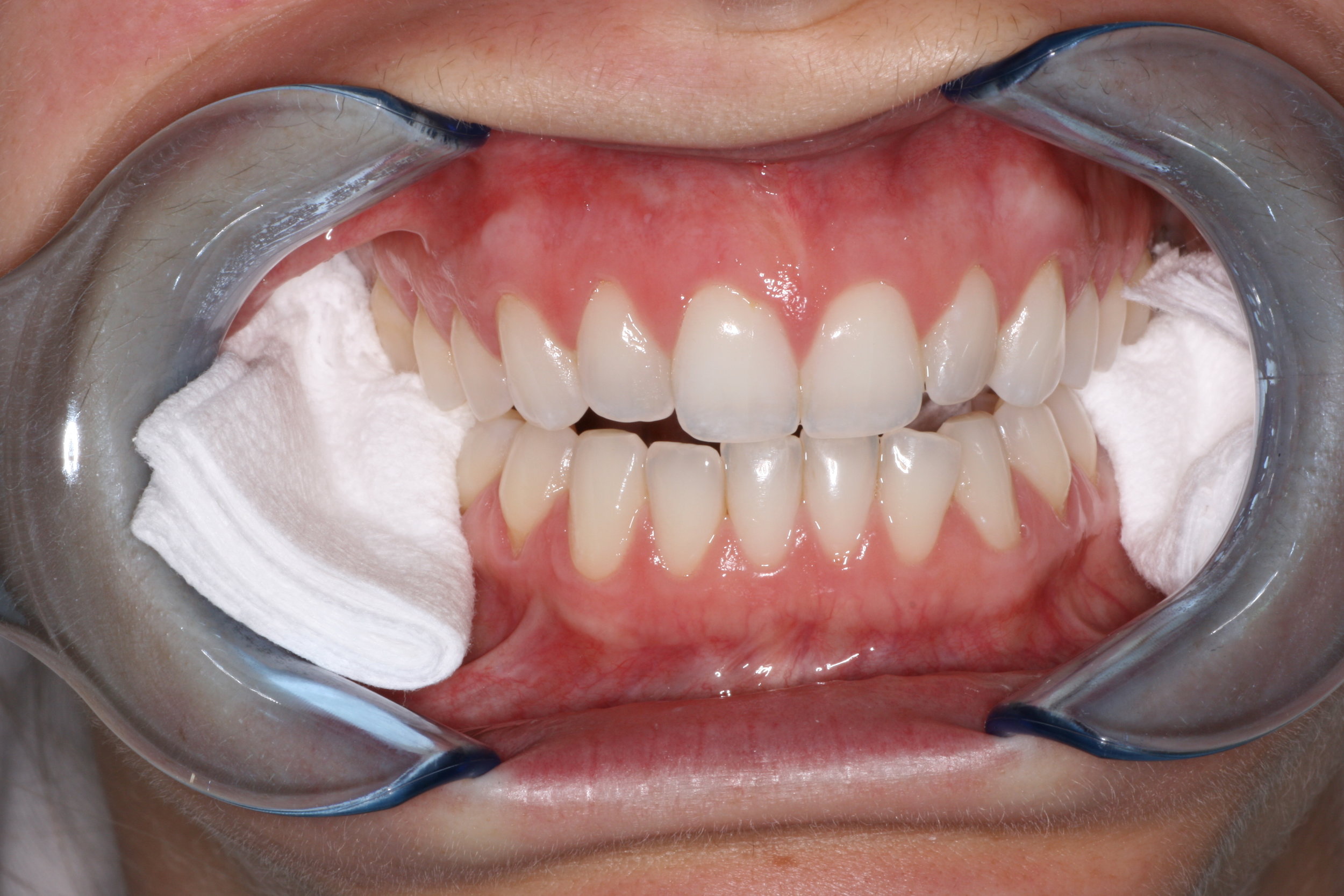
With tip of tongue on soft palate, bite on cotton rolls, 4 folded gauzes (2x2's) or most commonly on 2 folded gauzes placed on molars (keep off 2nd bicuspids). Goal is to record bite registration just inside freeway space anteriorly from second bicuspid to second bicuspid.
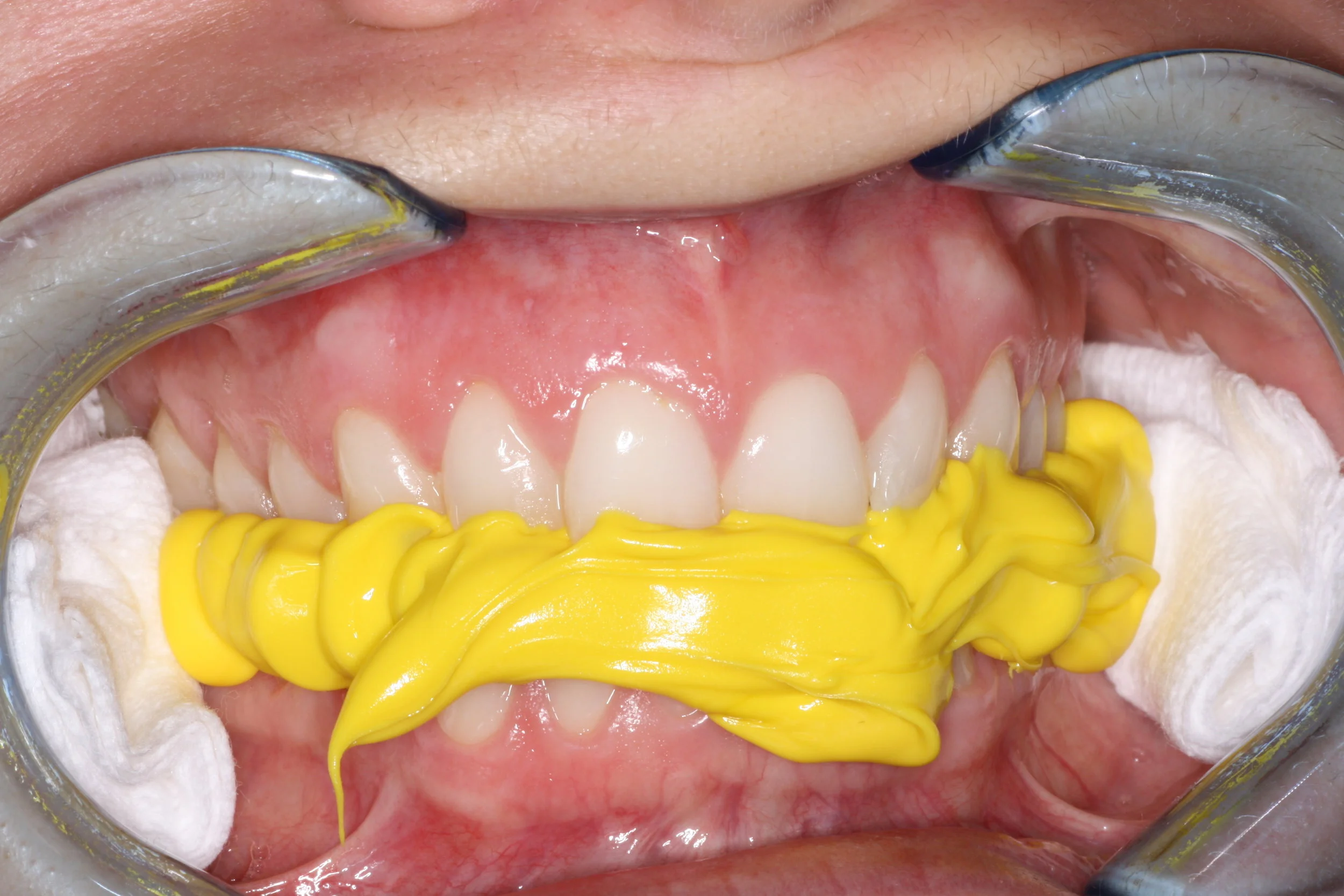
Using a stable bite registration material, record from 2nd bicuspid around to opposite 2nd bicuspid.
1. When inserting the MAPA; look for comfort, accuracy and proper retention. Good impressions will have assured this.
2. Next, have the patient bite on the MAPA's cuspid discluding platforms. The object is land both mandibular cuspids bilaterally and simultaneously on the cuspid pads of the MAPA when the condyles are in place (centric relation). Chances are you will need to do some minor adjustments on the discluding elements to achieve this. It is very important the contacts are equal in pressure when the condyles are in CR. To make sure they are closing in centric relation, you may do a Dawson “Romancing the Mandible” technique or you may have the patient touch the soft palate with the tip of their tongue while “pretending” to bite on their second molars or most posterior teeth. Do not let them use their own casual bite because their muscles and jaw relationships are usually problematic at this time and may give you highly inaccurate information. Avoid the patient protruding or going laterally when you are trying to create the correct orthopedic relationship between the mandible and the rest of the head with the MAPA in place.
3. If the opposing cuspids (either) are below the height of the neighboring incisors, having the cuspids land on the discluding element is difficult. In such a case, the lab may make a second appliance with artificially heightened cuspids to function against the cuspid pads. The freeway space still should not be violated but it may be close. Anterior open bites may have tall cuspid discluding elements to achieve function. Discluding elements designs are based on function and not symmetry.
4. When centric relation has been captured with balanced cuspid contacts, then have the patient protrude on articulating paper while keeping the cuspids on the cuspid pads until incisors are end to end either visually in space or in direct contact. Adjust the MAPA until the protrusive paths are equal in pressure and are straight. You may have to guide the mandible with your hand to help insure the mandible is moving straight while adjusting. Once properly adjusted, they should protrude straight without your assistance. Make sure no posterior teeth touch when protruding while traveling edge to edge. Most patients will never go past edge to edge incisally so posterior contact after that may not be critical.
5. Finally, have the patient go “straight” left and right for their lateral movements from the CR position. Adjust to make the pathways smooth and level, or relative so. Again make certain no posterior teeth touch in these excursions.
6. In the event you have posterior teeth touching in protrusion or in lateral, you may adjust the teeth to free these contacts or increase the height of the cuspid pads on the MAPA. Increasing height can easily be done using TRIAD bonding adhesive and its composite tray material, or something similar. Four millimeters is ideal for protrusive and lateral movements, but may be impossible in some cases.
7. When finished, polish the occluding surfaces of the pads only. You can also coat the pads with DuraFinish composite glaze. Use the “halogen only” cure product from Parkell. Stock No. S295.
8. Instruct the patient on how the MAPA works. Then discuss when to wear and how to clean it. Denture cleaners work well. Tooth brushes can scratch. Give the patient a handout reviewing what you said. The patient handout has excellent information on sleep, posture, hydration, etc.
9. The patient should wear the MAPA out the door, so do not forget the case.
10. The MAPA should be worn full time for six weeks (give or take two), except to eat and clean. It becomes bedtime wear after that. Some cases may require full time wear for a longer time period. During this time, two therapies should be accomplished starting two weeks after delivery followed by two or three week interval appointments after that. Bedtime wear may be indefinite for many and usually starts after three therapy appointments are completed. Therapy usually includes equilibration to create a stable and functional dental relationship with the TMJs. Muscles are being relaxed and returned to their normal working length. Other therapies, when needed, will be based on your training, equipment or on referral to a physical therapist, etc.
11. If the MAPA is used as a protector of dental work, then bedtime wear is all that is necessary. The MAPA is much more comfortable, works better and doesn’t wear out like so many other full arch protectors. The MAPA quickly becomes a “want to” rather than “have to” appliance to wear at bed time while protecting expensive dental work. Think of it as forcing normal on your patients while preventing trauma. Simply avoid posterior contact while keeping contact within the resting or freeway space.
12. Work with a good physical or massage therapist to help educate the patient on proper work, sleep and daily postures as they relax (regain normal working length) neck and shoulder muscles. Eliminating the trigger points within these muscles is necessary. Beware of therapist who only do hot packs and exercises. The neck and shoulder muscles are over exercised already and trying to relax them when trigger points are present by doing strengthening exercises make them worse. The object is to take tight muscles and return them to their normal working length. Caution your patients to never use dry heating pads. Moist heating pads are OK. A combination of 200 to 400mg of ibuprofen combined with 500 to 1000mg acetaminophen every 6 hours gives the best pain relief (providing these medications can be taken by your patient). Caution your patient on long term use. Never use narcotics, Ultram or Tramadol as they inflame glial cells surrounding nerves making the situation worse. Soma or Carisoprodol is a good muscle relaxer to use only at bedtime (no hang over like Flexaril). Do not use Soma for more than 30 days. Topical analgesics like Aspercreme applied to neck, shoulder, TMJs and jaw muscles make a significant impact in some patients. Cold is usually a distracter only and should never be used for more than a few minutes. Cold spray and stretch, however, can help the dentist when stretching a tight muscle to regain its working length.
13. Make sure the patient has the “Helpful Hints for Wearing The MAPA” handout. Reviewing it with them (or have an assistant review it with them) will greatly benefit the patient. Be prepared to answer patient questions.
14. Personal contact with Dr. Crout can be addressed to: drcrout@gmail.com.
Post note: Patients with deep overbites with traumatic fremitus will not improve until the lower incisors are equilibrated slightly out of contact.
Taking Care of Your Bite Guard
Your bite guard is a very important part of your therapy. It must be worn properly to achieve full results. Attending dental therapy appointments is also important.
The MAPA is nearly invisible and speech is usually no problem after the 2nd day.
Initially, you should wear your bite guard full time except to eat or clean it. You may drink with it in place. Bedtime wear only usually begins after the second therapy visit, but your dentist will tell you when to begin bedtime wear “only”. Speech and aesthetics are rarely problems. Long term wear will be established by your dentist, but many patients choose to wear this bite guard indefinitely at bedtime since most damage is done during sleep.
To clean the MAPA, soak it in Efferdent or Polident (15 minutes usually) or a similar product. Use cold or lukewarm water since hot water may warp it. Soaking longer should not harm the appliance. You may use mouth rinse for quick freshening. Do not use a toothbrush because it will scratch your bite guard.
Eating: When you take your bite guard out to eat, always put it back in the case to avoid losing it. CAUTION: Dogs love bite guards.
Try not to purposely bite or play with your bite guard but human curiosity says you might for a day or so. Most people do not notice they are wearing it after 10 days.
The MAPA Establishes Your Best “Jaw Fit”
When you take your bite guard out to eat, you may find your teeth not fitting properly for a few minutes. You lose the memory of your best “teeth fit” momentarily. The bite guard is matched to your best “jaw fit” (muscles and TMJ fit). Part of your therapy will be creating a stable and physiologic bite and jaw relationship. This may be done by minor equilibrations or adjustments to your teeth as your muscles relax. The adjustments rarely exceed the width of a hair on any selected spot. You should not visually see the difference before and after the adjustments, but your muscles and nervous system will certainly appreciate the change (improved function and stability).
Bite Guard Therapy
The MAPA functions quite differently from most other bite guards. This is good because it works in harmony with your body. It is a true neuromuscular device. First of all, it is passive. It fits within your resting jaw space (when your lips are together and your teeth are apart). Jaw muscle contractions happen when your teeth touch something or each other, such as in clenching. The message for your muscles to flex is integrated into the proprioception nerves around the roots of your teeth. Like an electrical switch, if there is no (tooth) contact, there is no electrical flow. Muscles relax (are not contracted) and return to their normal working length as a result. Teeth that have been intruded or pushed latterly from clenching will have a chance to seek their neutral position (those not covered). Orthopedic stability is achieved by muscle relaxation, your TMJ disc returning to proper position and by teeth returning to their normal unstrained position. Equilibration may be necessary to maintain neuromuscular function and harmony. Tooth adjustments occur on the sides and cuspal inclines of teeth and rarely on the vertical. In other words, your teeth are not “ground down” or made shorter.
Your Home Work
Proper posture when sitting, standing, or sleeping is very important. Sleeping on your stomach or with hands on your face with your neck twisted contributes to impingement of your airway and vertebral arteries. This can lead to lowered oxygen saturation which makes the brain irritable. This in turn can lead to bruxism. Lowered oxygen saturation to the brain accounts for much of our restless sleep. Restless sleep and vertebral artery (feeds the brain stem) impingement reduces the amount of serotonin, norepinephrine and dopamine you produce. Thyroid levels can also be affected. TMD (TMJ) and sleep issues are highly associated. Avoid sleeping on your back if you are significantly overweight, have a large tongue, low soft palate or snore. Side sleeping with your head, neck and spine in a straight line is always good. Don’t use a tall pillow for back sleeping.
Texting, holding phones, holding a steering wheel high, reading in bed on your stomach or side, working on computers and carrying heavy purses can devastate neck and shoulder muscles. Remember, most muscle tension type headaches come from the neck and shoulders. If you have trouble correcting bad posture or habits, place a band-aide on one of your fingers as a constant reminder to break the habit. It takes 30-45 days.
Drink a minimum of 65 oz. water while keeping to a minimum dehydrating drinks such as coffee, tea, alcohol and sodas. Also note that any caffeine intake after 4:00PM or within six hours of bedtime whether it be from coffee, tea, soft drinks or chocolate can disturb sleep. Alcohol, such as a glass of wine before bed, will likely cause poor sleep.
Physical therapy to the neck, jaws and shoulders compliment bite guard wear. Physical therapy may be done in your dentist’s office or may be referred out. This therapy may involve electronic devices, trigger point injections, laser therapy as well as hands on physical therapy. Your dentist may recommend a chiropractor in some cases. Relaxation of neck, shoulder and jaw muscles is necessary to achieve maximum success by returning muscles back to their normal working length. It is extremely important that you wear the MAPA as a compliment to these other therapies.
Since teeth are supposed to touch during heavy lifting, DOT NOT wear your bite guard if you are weight lifting or lifting objects that require teeth bracing.
Avoid using dry heating pads. Moist heat is good. Cold is a distracter only. Never sleep on a heating pad. Twenty minutes is long enough with a moist heating pad. Wait two hours before repeating.
Should you have additional questions, please call your dentist.